by: Jason Becker, FANS Supervisor
It all started in February of 2020 while working at Wal-Mart, along with working here at [NMC Health]. In February, we were starting to hear about COVID-19 in the news, and how it was spreading through out China. Here at the hospital we were getting emails and updates as it was coming down. For me at the start, I had mixed feelings as to whether this was real. Or was this something of sort related to politics?

Then March came, and the pandemic occurred. Everyone came out to the store (Walmart), and bought lots of toilet paper, dish soap, laundry detergent, groceries and practically anything that was not bolted to the floor. As a supervisor there, we worked long days trying to stock and keep shelves full.
At that point, we were not mandatory on wearing face covers. Then it became mandatory here at the hospital to do so. Finally, first part of April it became mandatory for us to wear face coverings and have our temperature taken as we clocked in at the store.
During the spring and summer there were many times us associates at the store were finding ways and places to lower our face covering because it was hot. It was hot outside and hard to breathe with the face mask on.
Through the summer, the hours of stores changed, social distancing was pushed hard, washing hands, along with sanitizing every thing. But still, many had doubts on whether and how serious this virus really was. There was much controversy wherever you went.
Then fall came and the outbreak started getting more and more severe. Not just here, but everywhere around the state. By October, it all changed for me.
On September 25, 2020, I had taken a nasty trip and fall while I was out mowing. I got a nasty sore (ulcer) on my right ankle. By Sept. 27, the sore was red. I had a rash starting on my left ankle, in which I knew both right and left ankle started showing some characteristics of cellulitis.
On Oct. 1, I went to NMC Health Wound Healing & Hyperbaric Center and they cultured both my left and right ankle. They called four days later and said they were going to put me on [an antibiotic] due to light-to-moderate growth. Later that afternoon, I found out I was allergic to the medicine. The pharmacist told me to take caution because I could react to it. So, after I got off work at NMC Health Medical Center, I stopped by and picked up the medicine. I took the first dose, then went on home. Shortly after 1 a.m. on Oct. 6, I was awakened by massive headache, cold and hot chills, skin crawling (itching) and my body aching. I thought, “Great. I am reacting to the medicine.”
So, I toughed it out. Then, in the morning, I decided to go to work and try to shake off the reaction. I got to work at 7 a.m. As I got out of the car to go into the store, the ground started to spin. I then decided it was best that I call in sick. I am one that never calls in sick, but I did anyway.
I went straight to the emergency department at NMC Health Medical Center. It took me some time, but I was finally able to get out of the car and make it inside. I told them what just happened, and that I thought I was having a reaction to the medicine.
In the ER they said they would swab me for COVID-19 to make sure it really was a reaction to the medicine. After a short while, Dr. Windham came back and told me I was positive for COVID-19. I thought to myself, “Oh great, I have the start of cellulitis and now I am going to have to fight COVID-19.”
So, I left the ER and headed home to Salina. While driving, I called my wife and told her what happened. She packed her stuff and headed to her parents house to quarantine for 14 days. I also visited with Saline County Health Department.
On the morning of Oct. 7 around 5 a.m., I got up to use the restroom. On the way out, I leaned against our towel cabinet and held my head. I felt HORRIBLE. I swore my head was going to explode. I took one step into our hallway to go back to bed and I passed out onto the floor. I was out approximately 15 minutes. I woke up to laying on the ground with one foot under me, one foot out and couldn’t move.
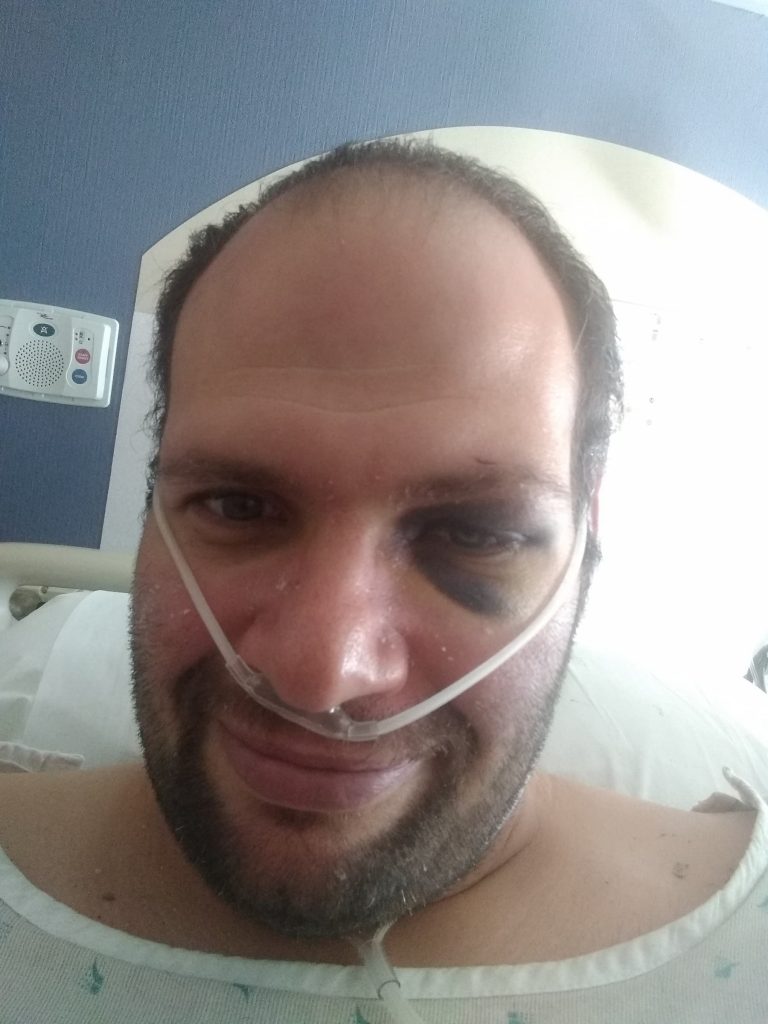
My head hurt and my eye was massively swollen. Luckily, I had my cell phone in my pocket so I called 911. Salina EMS came and they took me to the hospital. There, I had a fever of 102.3, and was severely dehydrated. They gave me fluids and broke my fever. Then, I had to call the Health Department to get clearance for my wife to come out of quarantine to take me home.
Three days later, I got up in the morning and went to the kitchen to make me some cereal for breakfast, but I was so weak that I couldn’t get the fridge or cereal cabinet open. I went and sat down in the recliner. Then around 2 p.m. I got up and thought I could at least open a soup can and have soup for lunch, but I was so confused and weak that didn’t happen either. So I grabbed a Gatorade and went and sat back down in the recliner. And there is where my life would change forever.
At around 5 p.m. my wife kept calling and calling and calling. Finally I answered. But I was as far to the left side of the plate as you could get it. She put me on speaker phone. She and her parents were asking me questions, but I just rambled on and made no sense. My wife told her parents they needed to get me some help right away.
She called 911 and explained to them what just happened. The dispatcher sent paramedics to our house. They came on in, and sure enough I was right there. I was rattling on talking. So, they loaded me up and rushed me to Salina Regional Hospital.
My wife and her parents came to the hospital, but due to COVID-19 restrictions, they were turned away and told they would have to talk to ER staff by phone. She advocated to the triage nurse about what was going on. She then waited and hour and a half for a doctor to call her.
She said that was the longest time ever, she had no idea whether I was alive or dead or what was going on. All she knew was that I was brought in by ambulance. Finally, the ER doctor called and they chatted. He told her they were going to give me liquids and then send me back home. My wife told doctor that she is in quarantine and that I would have to be able to take care of myself at home. ER doctor then said well that won’t happen called one of the hospitalists from 3rd floor (COVID floor) to come and check me out.
Dr. Humphrey came into the room where I was, asked me questions and I started rattling on, so he then ordered for a chest x-ray and lab work. He looked at my oxygen levels. I was on six liters of oxygen and my O2 saturation was in lower 70’s.
They came and did a chest x-ray first. A short time later, Dr. Humphrey and several nurses entered the ER room where I laid. They started working fast. Multiple IV’s were started, multiple poles were brought in and quite a few different bags were hung.
Then, a short time later, they started hitting me with shots in my arms and in my belly. There I was, confused as to what was going on. About three hours later (10 p.m.), I started coming to my senses. The doctor came in and said they were taking me up to the COVID-19 floor.
He said, “Thankfully we were able to start turning things around! Your chest x-ray showed your lungs are completely glassed over with COVID, and things are on the edge of shutting down.”
He said your chest x-ray showed your lungs are completely glassed over with COVID and things are on the edge of going to shut down.
About an hour after getting to my room on the COVID floor, the nurses called Dr. Humphrey to my room. He told me my body didn’t like the steroids I had just gotten down in the ER.
He said, “We know your not a diabetic, but the steroids have gotten your glucose level to 750.”
They started giving me insulin every hour until my blood sugar came down.
The next morning (Oct. 11), they changed my diet to 1500 calories a day, no more than 75 carbs a meal. And from that point on, they gave insulin while I was on massive steroids and oxygen. Also Dr. Humphrey came in and talked to me all of what happened the night before. He said besides your lungs being glassed over from COVID, your labs also showed you were septic.
As for the first hospital visit, I spent nine days in the hospital. While there, I had to have respiratory therapy, occupational therapy, physical therapy, insulin therapy, and oxygen therapy.
Two days before getting out of the hospital, I started having problems swallowing and so Dr. Nguyen came and started me on what they called swizzle. It is a four-compound medicine that would numb my esophagus so that I could eat and swallow. I was released from hospital on Oct. 19.
Six days later, on the morning of Oct. 25, a blood vessel broke in my ankle causing me to have to go back to Salina Regional by ambulance. There they treated the blood vessel and got the bleeding to stop. Then, I was sent back home.
While at home all afternoon I was light headed and really dizzy. So, finally I went and woke up my wife and told her we need to go back to the hospital. She came and sat down on the couch and we talked about what was going on. I said my pulse is rapid running 140-150 with me sitting and every time I get up I am light headed and feel like I am going to faint and pass out.
I told her we need to go and see if I am anemic from the blood loss in the morning. So she helped me out to her car, and back to Salina Regional ER we went. There, they did an EKG and blood work up. The doctor ordered for me to have a CT scan done. Shortly after coming back from the CT scan the ER doctor came in to talk to me and my wife.
He look at both of us and said, “I do not have one bit of good news for you.”
I looked at my wife and back to the doctor.
He said, “You have a pin hole in your lung leaking air. You have air pockets all over your chest cavity, and around your heart. You also have a VERY large blood clots. ONE clot in each lung.”
He said, “This is part of post COVID,” and told us this is what a lot of people die from after having COVID.
He said, “We are going to admit you for observation and start you on high doses of Eliquis to try get blood clots to dissolve. A surgeon will come see you the next morning and discuss what will need to happen.”
On the morning of Oct. 26, the surgeon came in and told me I would be staying a couple of days while they got me started on a heavy dose of blood thinners. She explained that I would not be able to cough, strain or lift for a while, because it could cause the clots to break and end up moving up to my heart or brain.

I got out of the hospital on Oct. 27. On Oct. 29 at 12:30 a.m., I was on the phone praying with my cousin. All of a sudden I got into a coughing fit. I could not stop. Suddenly, the whole left side of my body was numb and tingling. Something was definitely wrong. I told my cousin what happened.
She said, “Lets hang up and you call your wife’s parents and have them take you to the hospital.”
So I did. My father-in-law came. On the way there, I called my wife at work to let her know what was going on. We got to Salina Regional ER and right away the triage nurse started taking me back in a wheel chair. While heading to the room she was on her phone and told whoever she was speaking with to pull the “stroke alarm”.
So, upon entering the room there were nurses, a person with EKG machine, lab people, and a doctor. They all start working on me. They ran tests for about an hour. Then they send me down for a CT scan.
At about 3:15 a.m., the ER doctor comes in and said “We are transferring you to Wesley Medical Center.”
She went on to say my D-Dimer was extremely high and that I was possibly having a stroke. So, I called my wife’s parents and they called my wife at work to get her to the hospital right away. They loaded me into the ambulance and hauled me to Salina Regional Airport where they loaded me into the back of the Life Save Airplane and flew me to Wichita Jabara Airport.
From there, they took me by ambulance to Wesley Medical Center. When I got there, they ran tests and came to the conclusion I had suffered a “mini TIA stroke.” I spent about three-and-a-half days there, and then was released to do rehab at home.
My wife became a caretaker and had to still work full time. She spent many days up all day and very few hours of sleep before working all night. It took about two weeks to start being able to do things on my own.
Through all of this, my doctor says “I am a miracle survivor.” My PA at Axtell Clinic says to me after looking all the reports over, “People with what you went through would have had a funeral already, but you are still here!”
My reply is My Lord and Savior is not done with me yet here on Earth. I definitely have a different outlook on life. Every day we must take for granted as this day may be your last day here. We must live to the fullest. Since going thru all of this I have been diagnosed with what they call Post COVID Syndrome.
I still have chest pains, extreme fatigue, extreme body aches, head aches, jaw pain, brain fog, and the list goes on. Not every day does each one of those happen. I may have a week go by with nothing, and then one or two of those things will happen. Only one underlying every day symptom is the fatigue.

Also as the E.O.B’s have been coming in, we are over 400,000 dollars in medical debt. However between my primary and secondary insurances every thing so far has been paid in full except for a little under 300 dollars. Can you imagine someone not having insurance and goes through this? This would cause a lot of people to go under!
Could this be prevented? Yes!! How? By getting vaccinated, wearing a face mask at all times, washing hands, social distancing, not traveling on vacation, etc.
I WOULD ENCOURAGE EVERY ONE TO GET VACCINATED IF THEY CAN BE VACCINATED!! Also EAT healthy, take VITAMINS, take CARE of yourself!! PLEASE DO ANYTHING YOU CAN TO STAY WELL!!
Tell others, help educate others on how seriously and deadly this virus and disease is!!
